Home »
Current Treatments »
Orthopaedic Treatment of the Hip
Orthopaedic Treatment of the Hip
The word "arthritis" literally means inflammation of a joint.
Arthritis of the hip joint, one of the most commonly affected joints, makes simple
activities of daily living increasingly difficult. Arthritis symptoms include difficulty
with walking, arising from chairs, pain in the groin, buttock, thigh, or knee, and even
difficulty with sleeping, dressing, or having sex. Pain leads to limping. Eventually,
weakness of the muscles around the hip develops.
The mainstay of treatment for hip arthritis is conservative, and includes the use of
anti-inflammatory agents and physical therapy. When these modalities are no longer
effective, total hip replacement (THR) should be considered.
Hip Replacement Surgery
The development of THR is one of the most dramatic and successful events in orthopaedic
history, and remains one of the most successful of all medical developments of the
twentieth century. Since its inception by Sir Doctor John Charnley in England in the
1960’s, millions have regained the ability to walk.
It is imperative that the surgeon and patient have a realistic understanding of the
expected outcomes before deciding that hip replacement surgery is indicated. The patient
is first cleared for surgery by taking a battery of blood tests, x-rays, an
electrocardiogram, and a physical examination. If there is a specific medical problem then
a specialist is asked to render an opinion concerning whether surgery is reasonable. The
patient’s blood is banked for use at the time of surgery if necessary, thereby protecting
the patient from the possibility of blood-borne infection. Drugs that can cause bleeding
are stopped, including anti-inflammatory agents, aspirin products, or anti-coagulating
agents such as Coumadin, Plavix, Fragmin, or Lovenox.
The patient enters the hospital the morning of surgery where the correct side to be
operated on is verified. The anesthesiologist evaluates the patient and administers a
sedative. The surgery is generally done under spinal anesthesia except in the case of
pre-existing back problems or bleeding disorders.
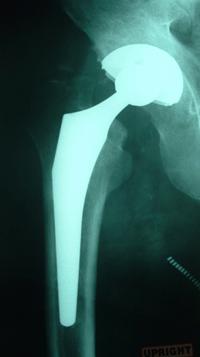
Once in the operating room, the old, damaged hip is removed. The new parts, made of
titanium, cobalt chromium, and other super metal alloys, as well as ceramic and/or high
density polyethylene type plastics, are carefully fit for size and position.
Some are cemented in place while most are press-fit, a newer technique.
After about one hour of surgery the patient goes to the recovery room until the anesthetic
wears off. The patient is usually walking the next day and discharged either to a
rehabilitation center or to home on the third day. At this time the patient is able to
walk with the assistance of a walker, crutches, or cane, go to the bathroom, and walk up
and down stairs. The patient will use an aid to walk for six to eight weeks.
Rare but possible complications include infection, blood clots, pneumonia, bleeding, nerve
injury, dislocation or loosening of the prosthesis, wear of the prosthesis, or leg length
abnormality. Precautions to avoid these possible complications are taken in every case.
Ninety percent of hip replacements last around twenty years, and some have lasted over
thirty. When hip replacements fail it is usually because of wear or loosening, depending
greatly on the weight and activity of the patient. THR is one of the most successful and
time-tested of all reconstructive surgical procedures.